Photos and Text Source: Hellenic Craniofacial Center (HCC). HCC was founded by the late Dr. Alexander Stratoudakis and is directed by Dr. Costas Alexandrou, Craniofacial Surgeon, Member of the Cyprus Center for Cleft and Facial Deformities, MEDICLEFT.#
Crouzon syndrome
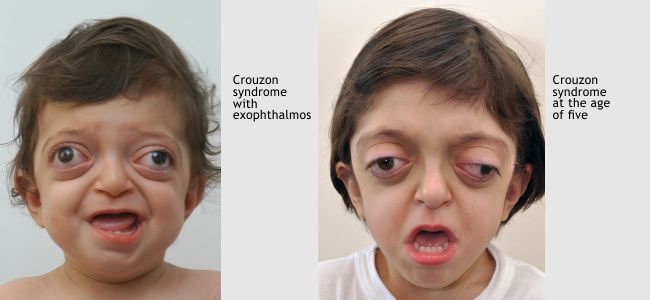
Crouzon Syndrome is characterised by multiple early synostosis of the sutures of the skull and face that derives its characteristic appearance.
Origin and Frequency
Crouzon syndrome is caused by multiple mutations in the FGFR 2 gene, which can be inherited from parents or are new mutations. The incidence of this syndrome is approximately 1:60,000 births.
Characteristics
Brachycephaly (short anteroposterior dimension of the head)
Facial hypoplasia
Exophthalmos that could lead, in severe cases, the eyelids not to close
Increased distance between the eyes (hypertelorism) usually in a non-serious degree.
The clinical picture varies from lighter form (which can elude diagnosis) to serious, incompatible with life.
Mental development
In most cases individuals with Crouzon syndrome have normal intellectual development.
Functional Problems
Increased intracranial pressure due to the reduced capacity of the skull. It’s a common problem and can appear at any time with serious consequences.
Decrease or loss of vision which is usually caused by increased intracranial pressure.
Eye irritation due to weakness in the closure of the eyelids. It can create permanent corneal damage.
Respiratory difficulty, especially during sleep obstructive sleep apnea). In severe form is incompatible with life. Even in the most mild forms it causes significant problems (disturbed sleep, sleepiness during the day, inability to concentrate).
Diagnosis Crouzon syndrome
It is diagnosed by physical examination and confirmed by gene identification. Gene identification is a lengthy process and becomes positive only about half of all cases, but that doesn’t matter because the confrontation of problems becomes the basis of the findings of physical examination.
Examination of a baby with Crouzon syndrome
Immediately after birth, clinical exam must be made for:
Respiratory function. If there is difficulty in breathing which continues after the initial support in the intensive care unit, possibly a tracheostomy is required.
Closure ability of the eyelids. If the baby cannot close his/her eyelids due to exophthalmous, a temporary tarsorrhaphy may be needed (the upper with the lower eyelid ) in order to protect the cornea until the permanent settlement of the problem.
Intracranial pressure. It is rarely needed to take immediate measures to correct it. The cases in which urgent surgery is needed are extremely serious and almost incompatible with life.
Surgical repair
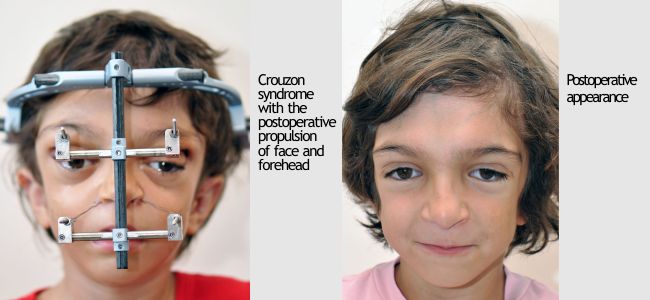
Because there is almost always a limitation of the capacity of the skull and the brain undergoes pressure, in infancy this pressure must be relieved with expansion (growth) of the cranial cavity. Usually the initial surgery is performed in the back area of the skull in parietal and occipital area (Parietal Decompression). A few months later (if necessary) decompression in anterior part of the skull follows (fronto-orbital advancement). In this intervention the area of ocular conches is formed and exophthalmos is somewhat reduced. Finally, at the age of 10-12 years complete and permanent correction of the deformity and the functional problems are achieved by transferring the anterior part of the skull and face forward with Distraction Osteogenesis (fronto–orbital advancement). This operation can be done at an earlier age, if necessary, due to functional problems that require immediate solution (obstructive apnea, increased intracranial pressure causing decreased vision).
Photos show patients had been operated by the late Dr. Alexander Stratoudakis founder of the Hellenic Craniofacial Center (HCC). and co-founder of Craniofacial Surgeon, Member of the Cyprus Center for Cleft and Facial Deformities, MEDICLEFT.
If you need any information about the treatment of clefts and other facial deformities, please contact + 357 25735050 or send us an e-mail at [email protected].
We will be next to you throughout the treatment procedure…
Photos and Text Source: Hellenic Craniofacial Center (HCC).